Green grasses are rich in precursors of vitamin E. Our cows graze pasture grass that is rich in Vitamin E. Vitamin E is a fat soluble vitamin and stays with fat portion of the milk. You can buy our products with confidence and at reasonable price.
Article written by Tina Beychok originally for: http://www.chiroeco.com/discovering-vitamin-d/75096/ The early 1900s diet
At the turn of the 20th century in western countries, it was believed the average diet should be 12 percent protein, 5 percent mineral, up to 30 percent fat, and up to about 50 percent carbohydrates.1 As can be seen, there is a heavy reliance on fats, proteins, and carbohydrates, with little focus on vitamins. Couple this diet with poor working and living conditions for the lower class, and it is not surprising that many people were extremely deficient in vitamin D. Industrial Revolution Such deficiencies lead to rickets, a condition in which the bones soften because there is a lack of vitamin D to help calcify them.2 As a result, the legs often bowed outward, and there were known to pain in the pelvis, spine, and legs.5 During the Industrial Revolution, poor children working in factories were most vulnerable to rickets.3 They often worked up to 14 hours a day, seven days a week. In addition to the dangers of being around large, heavy equipment, these children never were outside long enough to soak up the sun’s rays. Discovery of vitamin D Sir Edward Mellanby, a British researcher, came to be credited with some of the first discoveries of the nature of vitamin D. He fed dogs kept exclusively indoors a diet high in oatmeal, similar to that found in Scotland at the time. The result was that the dogs developed rickets.1 Mellanby correctly deducted that some substance in the oatmeal diet was linked to rickets. He found that cod liver oil cured the rickets, so assumed that vitamin A was responsible. Elmer McCollum and Marguerite Davis, American researchers, were interested in Mellanby’s findings. McCollum and Davis had previously discovered vitamin A, and by bubbling oxygen through cod liver oil, they were able to destroy the oil’s vitamin A. The oil still managed to cure rickets with vitamin A removed, and he was able to definitively determine is was not vitamin A but a new substance. They called it vitamin D.1 Milk fortification By the 1950s, most people thought that rickets had pretty well been eliminated, but in Canada there was a marked increase in cases of vitamin D deficiency seen in hospitals after fortification of milk was stopped. The government promptly re-introduced milk fortification.4 In Great Britain, an outbreak of hypercalcemia, or too much vitamin D, led the government to strictly reduce vitamin D fortification only to cereals and margarine.4 Research for determining the correct doses of vitamin D for adults, children, and infants is ongoing. Today’s vitamin D Symptoms of vitamin D deficiency today include metabolic disorders, cancer, cardiovascular disease, autoimmune diseases, infections, depression, and cognitive disorders.6 All milk sold in the United States and Canada is now voluntarily fortified with vitamin D. Other foods often fortified include margarine and yogurt, and most Americans get their vitamin D intake from fortified foods.7 In today’s modern, industrialized society, it is often too easy to assume that vitamin-enriched foods have always been there. The truth is, as with any other scientific discovery, it takes time to make all the connections necessary to understand how vitamins affect our body. This is certainly the case with vitamin D.
Rickets, a disease caused by a lack of calcium and vitamin D that leads to softening of the bones and bone deformities is reportedly on the rise in the United States and elsewhere. Once the most common nutritional disease of children, Rickets caused bowlegs and other problems such as deformed pelvises. It was first vanquished by teaching mothers to give their infants and children cod liver oil and sunbaths, and subsequently with the vitamin D fortification of milk beginning in the 1930s. So, why has it come back and who is at risk?
People with dark skin have a higher risk, because they need more sunlight to get enough vitamin D. Also at risk are breastfed babies that to do not get vitamin D supplementation, young people who do not consume vitamin D fortified milk, people living in northern latitudes who miss effective sun exposure for parts of the year and others who get neither sun exposure nor vitamin D supplementation and calcium in their diets. Do you spend your time inside playing video games and drinking soda? You aren’t helping your bones. Cod liver oil and sunshine both provide vitamin D and both were recommended for preventing and treating rickets beginning in the 1920s. The United States Children’s Bureau as well as state and local health agencies began promoting both measures in the childcare advice pamphlets. The Children’s Bureau distributed the pamphlet “Sunlight for Babies” as well as “Baby’s Daily Time Card” meant to be hung near the crib. It listed times for sunbathing and when to administer the cod liver oil in orange juice. The Metropolitan Life Insurance Company gave advice booklets to its policyholders including one entitled, “Sunlight the Health Giver.” In winter, families were instructed to keep the baby inside in front of an open window, while manufacturers encouraged the purchase of windows with special glass that let in the sun’s helpful rays or the use of indoor sunlamps. For those without yards or time to watch babies take sunbaths, window cages were designed to hold babies safely out in the open air. Health experts, government agencies, and manufacturers also promoted giving infants and children cod liver oil. Like sunbathing, it had long been touted as having numerous health benefits, such as preventing anemia, colds, and even tuberculosis. Yet, babies and children hated the taste. The Children’s Bureau tacitly acknowledged this in the second edition of its booklet, “Infant Care,” when it advised: “The mother must not let him know by her facial expression that she does not like the smell of the oil because that will teach the baby not to like it. She must take it for granted that he will like it even if she does not.” Fat chance. As one mother wrote in her son’s baby book about teaching him to take barley water “at least we do not have to force it down as we do the cod liver oil, which he hates. Until his bath he has a strong fish odor for he spits the oil out usually and it gets in his sleeper.” Ironically, the success of the campaign to get mothers to give infants and children cod liver oil meant that generations of youngsters continued to be dosed with the foul-tasting and foul-smelling stuff even when they no longer needed it for preventing rickets thanks to the widespread availability of vitamin D fortified milk. That doesn’t mean cod liver oil (now thankfully available in pill form) doesn’t have its uses. It is now used for high blood pressure, heart disease, and diabetes, among other conditions. Vegetarian alternatives are available. Likewise, sunbaths are back; albeit in strictly limited amounts. The American Academy of Pediatrics recommends no direct sunlight for babies under six months of age and limited exposure after that and opposes altogether the use of tanning beds. According to the government, ten to fifteen minutes in the sunshine, three times a week, is sufficient to produce the body’s requirement of vitamin D.
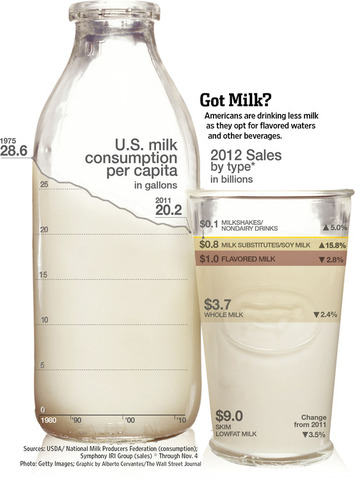
Per-capita U.S. milk consumption, which peaked around World War II, has fallen almost 30% since 1975, even as sales of yogurt, cheese and other dairy products have risen, according to U.S. Department of Agriculture statistics. The reasons include the rise in popularity of bottled waters and the concern of some consumers that milk is high in calories.
Click Images to Enlarge
TOPICAL APPLICATION OF COD LIVER OIL OINTMENT ACCELERATES WOUND HEALING: AN EXPERIMENTAL STUDY IN WOUNDS IN THE EARS OF HAIRLESS MICE 2000, Vol. 34, No. 1 , Pages 15-20 (doi:10.1080/02844310050160123) Louise Holmen Terkelsen, Anni Eskild-Jensen, Hanne Kjeldsen, John Howard Barker, Vibeke Elisabeth Hjortdal Institute of Experimental Clinical Research, Aarhus University Hospital, DK 8200 Aarhus N, Denmark The effect of topical cod liver oil ointment on the rate of wound epithelialisation and neovascularisation was studied using the hairless mouse ear wound model (experiment I). The effect of local application of vitamin A in increasing concentrations was tested in the same model (experiment II). Experiment I: Bilateral standardised full thickness dermal wounds were created on the ears of 42 mice divided into three groups: group I: 25% cod liver oil ointment (n = 10) applied topically to one ear and vehicle (vaseline) to the other; group II: 25% cod liver oil ointment (n = 10) and saline; and group III: vehicle (n = 22) and saline. Experiment II: Using the same model and procedures wounds were made on 12 mice randomised to vitamin A treatment in various doses (250-3000 IU/g) on one ear and vehicle (vaseline) on the other ear. Using in-vivo microscopy and digitised planimetry, wound epithelialisation and neovascularisation were measured at regular intervals until the processes were complete. Wounds treated with 25% cod liver oil ointment epithelialised significantly (p < 0.05) faster (mean (SEM) 8.9 (0.7) days) than control ears treated with vehicle alone (13.9 (1.9) days). Neovascularisation developed significantly faster (p < 0.01) in the ears treated with cod liver oil ointment (22.5 (1.3) days) compared with their vehicle control (29.1 (0.6) days). Neovascularisation was also significantly (p < 0.05) faster in the ears treated with cod liver oil ointment (23.1 (1.4) days) than in those treated with saline (26.8 (1.1) days). There was no significant difference in speed of epithelialisation between cod liver oil ointment and saline. The vitamin A dose study showed that epithelialisation and neovascularisation of the vitamin A treated wounds pass at the same rate as wounds treated with cod liver oil ointment. In conclusion, topical 25% cod liver oil ointment significantly accelerated both the epithelial and the vascular component of healing compared with saline. Vitamin A seems to have an important role in accelerating wound healing and could be the active component in cod.
Full Article |
Categories
All
|
© COPYRIGHT 2023 NutraPro International
Logan, Utah, USA
Logan, Utah, USA


 RSS Feed
RSS Feed